AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Pulmonary edema lung sounds2/25/2024  The activation of Rho via the action of its target protein causes phosphorylation of myosin light chains, actomyosin contraction and dysfunction of the endothelial barrier cells. 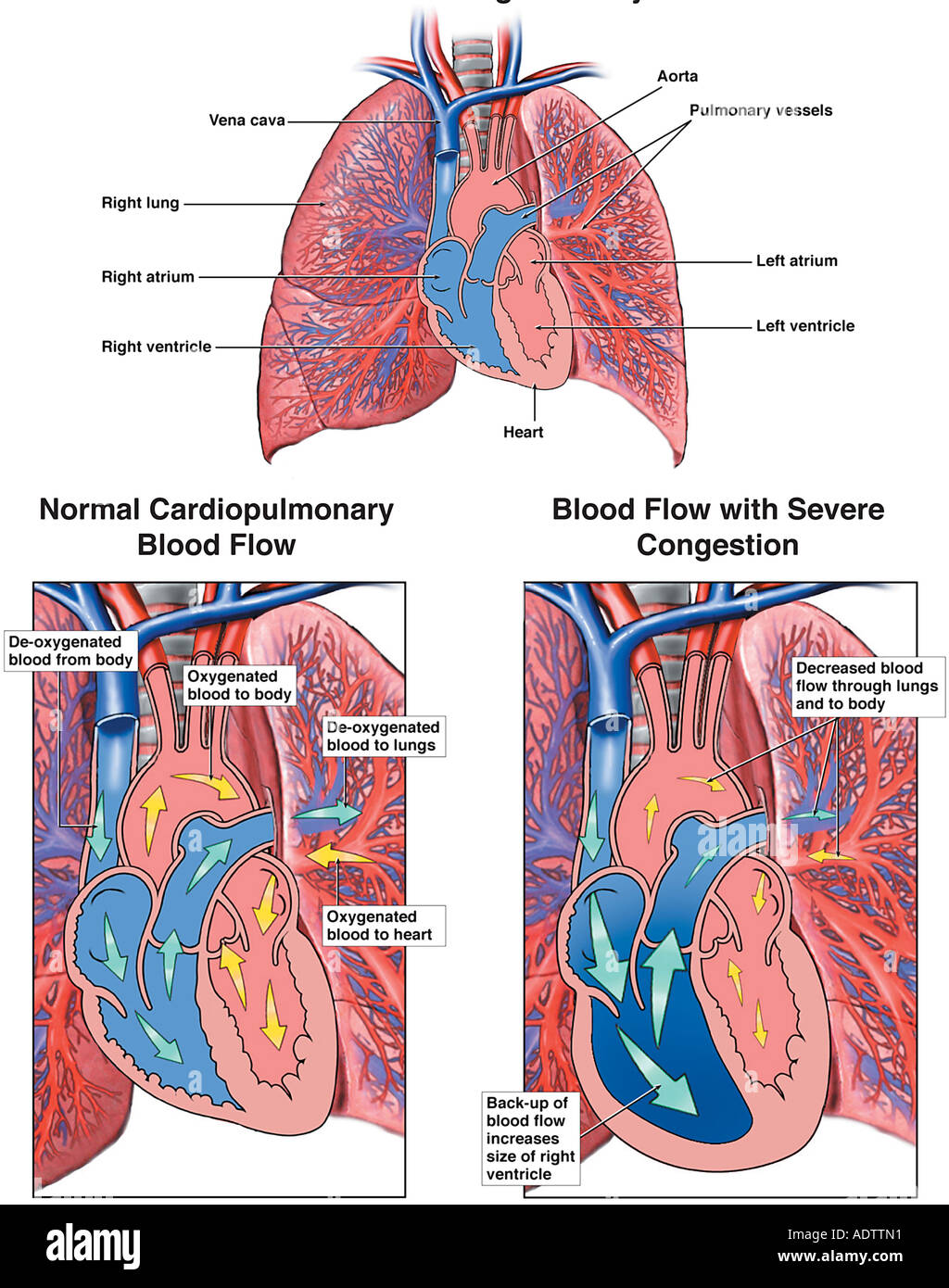
4 Another recent study identified a signaling pathway of the small guanosine triphosphate-binding protein Rho and its target protein ROCK (Rho-associated coiled–coil-forming protein kinase) as a possible mechanism. Inflammatory mediators, including interleukin 8, leukotriene B4 and monocyte chemotactic activating factor, are pivotal in this inflammatory response. Ventilation and reperfusion of a previously collapsed lung may lead to an inflammatory response, with production of reactive oxygen species and superoxide radicals, a sequence of events that ultimately results in increased capillary permeability. One of the more promising theories suggests that the root of the condition is increased permeability of the pulmonary capillaries as a result of inflammation. 3Īlthough the pathophysiology of re-expansion pulmonary edema is multifactorial and poorly understood, new investigations are uncovering possible mechanisms. Proposed risk factors include age between 20 and 40 years, 5 duration of collapse greater than 72 hours, the application of high negative pressures during thoracic drainage (> 20 cm H 2O), and rapid lung expansion with drainage of large volumes of pleural fluid (> 1.5 L). 3 A chest radiograph is usually diagnostic.Īlthough most patients completely recover within five to seven days, severe re-expansion pulmonary edema can lead to sequestration of large quantities of fluid in the lung, which may result in shock and possibly death. Occasionally, it may affect a single lobe or the contralateral lung, or it may be a bilateral process. The edema generally affects the entire re-expanded lung. 3 The cardinal signs are tachypnea, tachycardia, and crackles on the affected side of the lung as well as hypoxemia, which may be refractory to oxygen therapy. The onset of symptoms is usually within 24 hours, with 64% of patients having onset within 1–2 hours after lung re-expansion. Symptoms of re-expansion pulmonary edema include chest discomfort, persistent severe cough, production of frothy sputum and dyspnea. The following day, a chest radiograph showed a well-expanded right lung with no evidence of pulmonary congestion ( Figure 1C). Over the next few hours, the patient’s condition improved and the ventilation was stopped. 
We started noninvasive ventilation with bi-level positive airway pressure. A chest radiograph showed pulmonary vascular congestion over the entire right lung with both chest tubes in situ, consistent with re-expansion pulmonary edema ( Figure 1B). 
He was tachycardic and normotensive, a few scattered crepitations were heard on the right side, and the oxygen saturation was 89% (normal 93%–100%). Two chest tubes were inserted, and the endotracheal tube was successfully removed.Īn hour later, the patient had shortness of breath. Evacuation of the empyema and decortication through a right lateral thoracotomy resulted in complete re-expansion of the right lung with no parenchymal lung injuries. Thoracoscopy showed a multiloculated and fibrinous empyema, with entrapment of the right lower lobe. Preoperative bronchoscopy excluded endobronchial lesions. We scheduled a video-assisted thoracoscopic decortication and drainage of the empyema. Analysis of the pleural fluid, with cultures positive for Streptococcus pneumoniae, confirmed our clinical diagnosis of empyema. We made a preliminary diagnosis of pneumonia with empyema and started empirical treatment with piperacillin–tazobactam 4.5 g intravenously every six hours. After we drained 800 mL of fluid via thoracentesis, a repeat chest radiograph showed no change in the size of the effusion. A computerized tomogram of the chest confirmed a loculated pleural effusion with nodular infiltrates in the right lower and middle lobes, with no masses or lymphadenopathy. A chest radiograph showed a moderate pleural effusion on the right side ( Figure 1A). His liver and renal profiles were normal. Laboratory examination showed a low hemoglobin level of 103 g/L (normal 135–175) and an elevated leukocyte count of 18.0 × 10 9/L (normal 3.5–11.0) with 92% neutrophils. The rest of his physical examination was unremarkable. There was dullness to percussion over the right side of his chest that extended from the midzone to the base coarse crepitations and bronchial breath sounds were heard above the area of dullness. He was febrile (temperature 38.6☌), tachycardic, and dyspneic at rest. He had an eight-pack-year history of smoking with no significant medical history. A 24-year-old man was admitted with a two-day history of shortness of breath and right chest pain. 
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
